Third card, fourth shot
-
An impressive illustration of what it means to take immunosuppressants, especially if you consider that similar issues likely arise with actual viruses that are not vaccines.
-
Any word on whether certain vaccines work better for immunosuppressed individuals?
-
https://www.nejm.org/doi/full/10.1056/NEJMc2111462?query=featured_home
Randomized Trial of a Third Dose of mRNA-1273 Vaccine in Transplant Recipients
To the Editor:
In organ-transplant recipients, the standard two-dose vaccination strategy for coronavirus disease 2019 (Covid-19) has suboptimal immunogenicity.1 Both patients and health care providers have questioned whether a third-dose booster in transplant recipients would be safe and enhance immune response.2 We performed a double-blind, randomized, controlled trial of a third dose of mRNA-1273 vaccine (Moderna) as compared with placebo (the protocol is available with the full text of this letter at NEJM.org; ClinicalTrials.gov number, NCT04885907).
Transplant recipients who had received two doses of mRNA-1273 were randomly assigned in a 1:1 ratio to receive either a third dose of mRNA-1273 vaccine or saline placebo 2 months after the second dose of mRNA-1273 (dosing schedule: 0, 1, and 3 months). The primary outcome was a serologic response characterized by an anti–receptor-binding domain (RBD) antibody level of at least 100 U per milliliter at month 4 (measured with an Elecsys Anti-SARS-CoV-2 immunoassay [Roche]). This outcome was prespecified and was based on the protective anti-RBD titer in a challenge study involving nonhuman primates3; it was further corroborated in a large clinical cohort as the upper boundary of the estimated level required to confer 50% protective neutralization.4 Secondary outcomes included the percent neutralization, as measured with a validated surrogate virus neutralization assay (Genscript), and the polyfunctional T-cell response (see the Supplementary Appendix, available at NEJM.org).
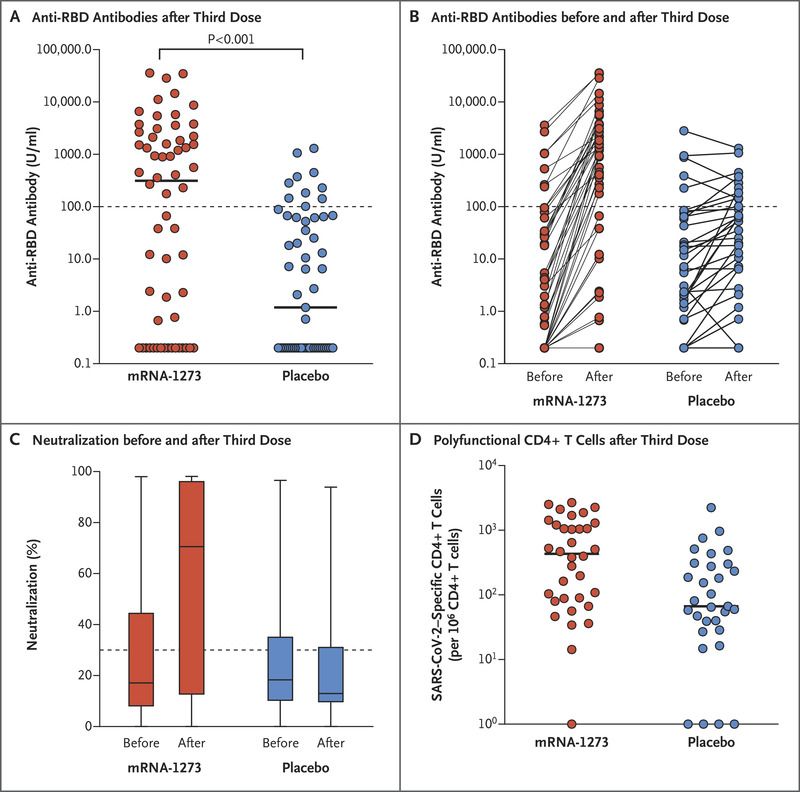
We enrolled 120 organ-transplant recipients (Fig. S1 in the Supplementary Appendix). No patient had a previous diagnosis of Covid-19. The baseline characteristics were similar in the two groups (Table S1), as were the preintervention anti-RBD antibody levels and neutralizing antibody levels (). The median age of the patients was 66.6 years (interquartile range, 63.3 to 71.4), and the median time from transplantation to the third dose was 3.16 years (interquartile range, 1.71 to 6.12). The time from transplantation was slightly shorter in the placebo group than in the mRNA-1273 group; however, the types, doses, and levels of immunosuppression were very similar in the two groups, as were the lymphocyte counts. Covid-19 developed in 1 patient (placebo group; preinfection anti-RBD antibody level, 75 U per milliliter), and 2 patients did not provide follow-up blood specimens.
At month 4, an anti-RBD antibody level of at least 100 U per milliliter was present in 33 of 60 patients (55%) in the mRNA-1273 group and in 10 of 57 patients (18%) in the placebo group (relative risk, 3.1; 95% confidence interval [CI], 1.7 to 5.8; P<0.001) ( and Table S2). The changes in anti-RBD antibody level from before to after the third dose are shown in . After the third dose, the median percent virus neutralization was 71% in the mRNA-1273 group and 13% in the placebo group (95% CI for the between-group difference, 11 to 76 percentage points), and the percentage of patients above the 30% threshold for neutralizing antibody positivity was 60% and 25%, respectively (relative risk, 2.4; 95% CI, 1.5 to 4.0) ( and Table S2). Median severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)–specific T-cell counts were greater after the third dose in the mRNA-1273 group than in the placebo group (432 vs. 67 cells per 106 CD4+ T cells; 95% CI for the between-group difference, 46 to 986) (). There was a minimal polyfunctional CD8+ T-cell response in both groups. In the safety evaluation, local and systemic events were slightly more common after the third dose of mRNA-1273 than after the dose of placebo (Fig. S3), but no grade 3 or 4 events and no cases of acute rejection occurred.
A third dose of mRNA vaccine in transplant recipients had substantially higher immunogenicity than placebo, as determined in our analysis of both primary and secondary trial end points. This trial had short follow-up and was not powered to detect differences in clinical outcomes. We also acknowledge that the cutoff value of 100 U per milliliter for the anti-RBD antibody level is arbitrary and is not necessarily predictive of resistance to infection. A third dose was safe when risk versus benefit was considered. We note that a small subgroup of patients who received placebo did have modest increases in antibody levels (). This may reflect ongoing mRNA vaccine–induced B-cell stimulation, as recently described,5 and highlights the importance of evaluating a control group. We conclude that a third-dose booster Covid-19 vaccine should be considered, in conjunction with regulatory approval, for transplant recipients who have received two doses of mRNA-1273.
-
Did they really need to run the test vs. a placebo? I don't see the benefit there. The only tests that really matters are the levels at shots 1, 2, and 3...
-
Did they really need to run the test vs. a placebo? I don't see the benefit there. The only tests that really matters are the levels at shots 1, 2, and 3...
@lufins-dad You need to confirm the intervention made the difference. What if, for example, antibodies just develop more slowly in immune suppressed people?
Hello! It looks like you're interested in this conversation, but you don't have an account yet.
Getting fed up of having to scroll through the same posts each visit? When you register for an account, you'll always come back to exactly where you were before, and choose to be notified of new replies (either via email, or push notification). You'll also be able to save bookmarks and upvote posts to show your appreciation to other community members.
With your input, this post could be even better 💗
Register Login
